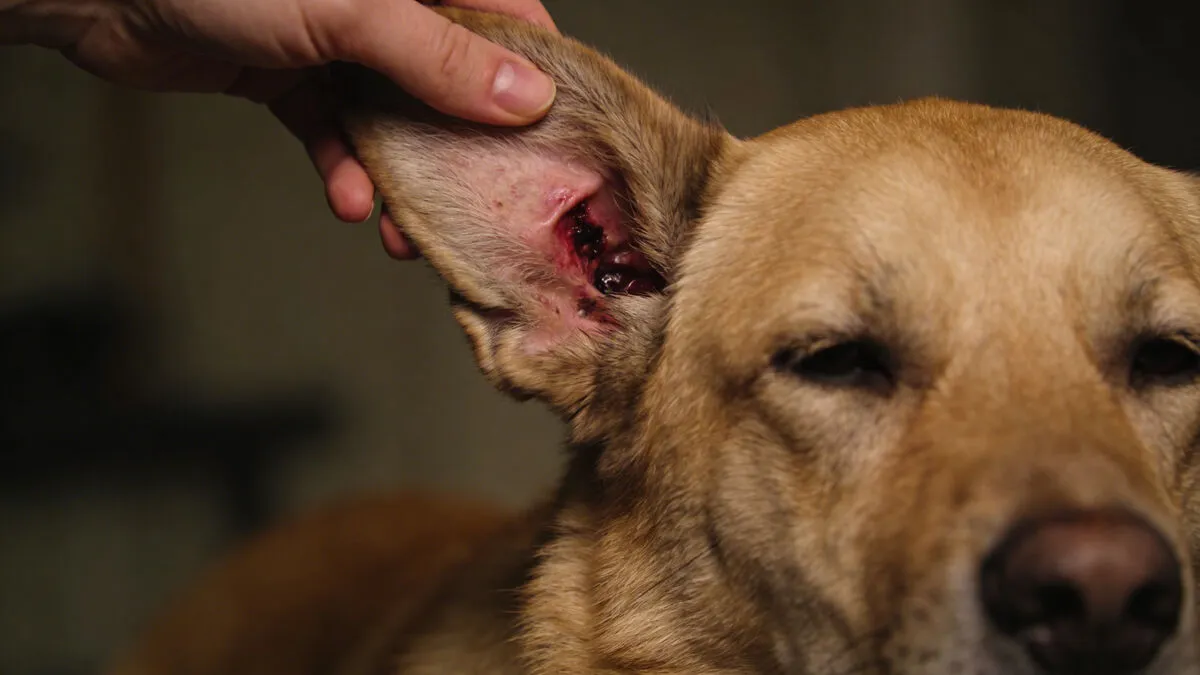
You've been through this cycle more times than you can count. Your dog's ears become inflamed — red, smelly, itchy. Your vet prescribes ear drops, possibly oral antibiotics or antifungals, possibly a steroid. The infection clears. Six, eight, ten weeks later, it's back. Same symptoms, same treatment, same temporary resolution.
At some point, your vet may have mentioned Apoquel, Cytopoint, or a referral to a dermatologist. What they may not have mentioned yet — or may not have explored in enough detail — is food.
Recurring ear infections are one of the strongest clinical signals of food sensitivity in dogs. Not the only cause. But a consistent, well-documented one.
Why Ears Are Such a Reliable Indicator of Food Sensitivity
The ear canal in dogs is structurally different from the human ear — it forms a distinctive L-shape, with a long vertical canal leading to a horizontal canal before the eardrum. This shape, combined with warm temperatures, limited airflow, and naturally occurring microorganisms, creates an environment that is exquisitely sensitive to systemic inflammation.
When food proteins trigger an immune response, the resulting systemic inflammation disrupts skin barrier function throughout the body — including in the delicate skin lining the ear canal. This disruption changes the microenvironment of the ear: pH shifts, the normal population of bacteria and yeast is disturbed, and the conditions that allow Malassezia yeast and bacteria to overgrow are established.
The infection that follows is real — it requires treatment. But it is secondary. The primary event is the inflammatory disruption caused by the food trigger.
The "Ears and Rears" Pattern: What It Tells You
Veterinary dermatologists have long recognised a clinical pattern so consistent it has its own shorthand: "ears and rears." Dogs with food-driven inflammation frequently present with two concurrent symptom clusters — recurrent ear infections (otitis externa) and rear-end symptoms including anal gland problems, perianal itching, scooting, and rear-end licking.
This pattern is not absolute — not every food-sensitive dog shows both. But when a dog presents with chronic ear infections alongside any rear-end symptoms, the probability that food is a contributing factor is high enough that it should be investigated before committing to long-term immunosuppressive medication.
Other common accompanying signs of food-driven inflammation include paw licking (particularly the interdigital spaces), facial rubbing, and generalised itching that does not follow a seasonal pattern. If your dog's ear infections occur year-round — not just during pollen seasons — food becomes a more likely contributor than environmental allergies alone.
Why the Infections Keep Coming Back Despite Treatment
The treatment your vet prescribes for an ear infection — antimicrobials, antifungals, steroids, ear cleaners — is appropriate. The infection is real and needs to be addressed. But the treatment targets the secondary event, not the primary cause.
Here is the cycle in full:
- A food protein triggers a systemic immune response.
- Inflammation disrupts the skin barrier throughout the body, including the ear canal.
- The altered ear environment allows bacteria and/or yeast to overgrow.
- A clinical ear infection develops — your dog shakes their head, scratches, the ears smell, discharge appears.
- Your vet treats the infection. It resolves.
- The dog continues eating the same food. The inflammatory trigger remains.
- The ear environment is disrupted again. Another infection develops.
Each cycle of infection and treatment can cause progressive changes to the ear canal — thickening of the skin, narrowing of the canal, increased wax production — that make subsequent infections more likely and more difficult to treat. In severe cases, chronic untreated otitis can lead to middle ear infections (otitis media), hearing loss, or the need for surgical intervention.
This is why identifying and removing the dietary trigger is not just about comfort — it's about preventing progressive ear disease.
The Delayed Reaction Window
One of the reasons the food connection is so frequently missed is timing. Food sensitivity reactions in dogs are not immediate. They are delayed — typically by 24 to 72 hours, and sometimes longer.
This means that the food your dog ate on Monday may not produce increased ear inflammation until Wednesday or Thursday. By that point, you've fed multiple other meals, and the connection between a specific food and the symptom flare is invisible without tracking.
It also means that when you switch foods and don't see immediate improvement, it doesn't mean the switch didn't help. Inflammation takes time to build, and it takes time to resolve. Skin and ear symptoms driven by food sensitivity can take 8 to 12 weeks to fully improve after the trigger is removed — far longer than most owners expect.
This delayed timeline is why so many owners who've "tried changing the food" conclude it made no difference. They were looking for a fast response to a slow process.
How to Investigate Whether Food Is Driving Your Dog's Ear Infections
If your dog has had three or more ear infections in a 12-month period, a food investigation is warranted — alongside (not instead of) veterinary treatment for any active infection. Here is a structured approach.
Step 1: Treat the Active Infection First
Do not attempt to diagnose a food trigger while your dog has an active ear infection. The infection produces its own inflammation and discomfort, which confounds any attempt to assess whether dietary changes are making a difference. Complete the full course of prescribed treatment. Wait until the ears are clinically clear before beginning the dietary investigation.
Step 2: Start a Strict Elimination Diet
The elimination diet remains the only validated method for diagnosing food sensitivity in dogs. Blood tests, saliva tests, and hair tests marketed for food sensitivity in dogs have been shown in multiple studies to produce unreliable results. The same is true for humans — read more in our carnivore elimination diet guide.
Choose a single novel protein — a protein your dog has never eaten before. Common options include kangaroo, venison, rabbit, or horse, depending on your dog's dietary history. Pair it with a single novel carbohydrate if needed (sweet potato, for example, if your dog has never had it). Feed nothing else — no treats, no chews, no flavoured supplements, no table scraps. Even small exposures to a trigger protein can sustain the inflammatory response and invalidate weeks of effort.
A true elimination diet should be single-ingredient: one protein source plus bones and a small amount of organs from the same species. Avoid ultra-processed commercial "elimination" diets — they contain multiple ingredients your dog could be reacting to beyond just the protein.
Step 3: Commit to the Timeline
An elimination diet for ear-related symptoms requires a minimum of 8 weeks, and ideally 10 to 12 weeks. Skin and ear symptoms resolve more slowly than gastrointestinal symptoms. Abandoning the trial at week 6 means you may miss the improvement that would have become apparent at week 9 or 10.
Step 4: Track Daily
This is the step that separates a useful investigation from wasted effort. Every day, record:
- Exactly what your dog ate — every meal, every treat, every supplement, every flavoured medication.
- Ear condition — redness, smell, discharge, head shaking, pawing at ears. A simple severity scale (0 = clear, 5 = severe) works well.
- Other symptoms — scratching, paw licking, rear-end licking, skin condition, stool quality.
- Any accidental exposures — food stolen from the counter, another pet's food, a treat from a well-meaning visitor.
This record is what allows you — and your vet — to see whether the diet is producing change, and if so, when and how much.
Step 5: Reintroduce One Protein at a Time
If your dog's ears improve significantly during the elimination phase, the next step is controlled reintroduction. Add back one protein at a time, feeding it daily for 1 to 2 weeks while continuing to track ear condition and other symptoms.
If a reintroduced protein triggers a return of ear symptoms — typically within 3 to 14 days — you have identified a trigger. Remove it, wait for symptoms to resolve, then test the next protein.
This process is slow. It can take months to test multiple proteins. But it produces specific, actionable answers about what your individual dog can and cannot tolerate.
Step 6: Build a Long-Term Diet Based on What You've Learned
Once you've identified which proteins trigger ear inflammation and which are well tolerated, you can build a sustainable long-term diet. This is the point at which the recurring infection cycle breaks — not because you've found a better ear treatment, but because you've removed the inflammatory driver that was creating the conditions for infection in the first place.
Which Dog Food Ingredients Are Most Likely to Cause Ear Infections?
If your dog has recurring ear infections driven by food sensitivity, there is a specific question you need answered: which protein is causing the problem? Research gives us a clear starting point.
Every dog is an individual. The ingredients listed below are the most statistically common triggers across the research — they are not universally "bad" foods. Two dogs in the same household can respond completely differently to the same protein. One dog may thrive on chicken and beef while the other reacts to both. The only way to know what affects your dog is to test systematically and track the results.
A comprehensive review of published studies on adverse food reactions in dogs (Olivry & Mueller, 2019) identified the most commonly reported trigger proteins, in order of prevalence:
- Beef — the single most frequently identified trigger in dogs with food-related skin and ear symptoms.
- Dairy — including cheese, yogurt, and milk-based treats. Many owners do not realise that the occasional cheese treat or pill pocket counts as a dairy exposure.
- Chicken — present in the majority of commercial dog foods, treats, dental chews, and flavoured supplements. Because of its ubiquity, chicken is both one of the most common triggers and one of the hardest to fully eliminate.
- Wheat — one of the few non-protein triggers that appears consistently in the literature.
- Soy — often present as a filler or protein supplement in commercial foods.
- Lamb — once considered a "hypoallergenic" protein, lamb has become a common enough ingredient in commercial foods that sensitisation rates have increased.
These ingredients are not inherently harmful. They appear at the top of this list because they are the most commonly fed — and exposure frequency drives sensitisation. A dog cannot develop a sensitivity to a protein it has never eaten.
It is worth noting that any protein can theoretically become a trigger. The six listed above are statistical frontrunners, not an exhaustive list. Some dogs react to less common proteins like pork, egg, or fish. The only way to identify your dog's specific triggers is through a controlled elimination diet with consistent tracking.
The "Grain-Free" Misconception
One of the most common responses to a dog with recurring ear infections is to switch to a grain-free food. While well-intentioned, this rarely solves the problem — because the trigger is almost always a protein, not a grain. A grain-free chicken-and-sweet-potato food still contains chicken. If chicken is the trigger, removing the grains changes nothing.
Similarly, switching from one chicken-based food to a different chicken-based food — even a "premium" or "limited ingredient" version — does not remove the trigger protein. The brand and price point are irrelevant. What matters is the specific protein your dog is reacting to.
What to Feed a Dog With Ear Infections
There is no single "best dog food for ear infections." The right food depends entirely on which proteins your individual dog can and cannot tolerate. Anyone claiming a specific brand or formula is the universal answer is oversimplifying a problem that requires an individual solution.
That said, there is a clear approach that works.
Start With a Novel Protein
A novel protein is one your dog has never eaten before. Because your dog's immune system has had no prior exposure, it has not had the opportunity to develop a sensitivity to it. Common novel protein options include:
- Kangaroo — rarely used in commercial dog foods, making it a strong novel option for most dogs.
- Venison — a common choice, though it appears in enough commercial foods now that some dogs may have prior exposure.
- Rabbit — another genuinely novel option for most dogs.
- Horse — used more commonly in European elimination diets.
- Duck — suitable if your dog has not been fed duck-based foods or treats.
Keep It Single-Ingredient
The most reliable elimination diet is single-ingredient: one protein source plus bones and a small amount of organs from the same species. No mixed-protein foods. No commercial "limited ingredient" formulas that still contain five or six ingredients beyond the primary protein. The simpler the diet, the clearer the signal.
Fish as a Common Safe Option
Fish — particularly species like sardines, mackerel, and whiting — is worth special mention. Many dogs have had limited prior exposure to fish proteins, making it a genuinely novel option. Fish also provides high levels of omega-3 fatty acids (EPA and DHA), which have documented anti-inflammatory properties that may support skin and ear health during the recovery period.
Fish is not universally safe — some dogs do react to fish proteins — but it is a strong starting point for many elimination diets, particularly when other novel proteins are unavailable or impractical.
Why Hydrolysed Diets Are Not Ideal
Veterinary-prescribed hydrolysed protein diets break proteins into fragments small enough that the immune system may not recognise them as triggers. In theory, this allows any protein source to be used safely. In practice, some dogs still react to hydrolysed diets — either to residual intact proteins or to other ingredients in the formula. Hydrolysed diets also tend to contain multiple ingredients beyond the protein source, which makes it harder to identify the specific trigger if symptoms persist.
A single-ingredient novel protein diet provides clearer information. If symptoms resolve, you know the novel protein is safe. If they persist, you know to investigate further — without wondering which of eight ingredients in a hydrolysed formula might be the problem.
What to Avoid During an Elimination Diet
- Multi-ingredient commercial foods — even "limited ingredient" formulas typically contain more ingredients than the label emphasis suggests.
- Treats and chews — rawhide, dental sticks, pig ears, bully sticks, and flavoured chews all contain proteins that can sustain an inflammatory response.
- Flavoured medications and supplements — many are flavoured with chicken or beef. Ask your vet about unflavoured alternatives during the elimination period.
- Table scraps — even small amounts of a trigger protein can restart the inflammatory cycle and invalidate weeks of dietary discipline.
- Other pets' food — if you have multiple animals, ensure your dog cannot access their bowls.
The Answer Comes From Your Dog's Data
No article, no vet, and no food manufacturer can tell you which specific protein is safe for your specific dog. The answer comes from tracking — logging what your dog eats every day and monitoring ear condition, skin symptoms, energy, and digestion over weeks and months. The patterns that emerge from consistent tracking are what transform a guess into a confirmed answer.
Start tracking your dog's food and symptoms — it takes under two minutes a day, and the data accumulates into something your memory alone cannot replicate.
Breed Predispositions Worth Knowing
Certain breeds are predisposed to both food sensitivity and ear infections, often due to a combination of genetic immune tendencies and ear anatomy. Breeds with long, heavy ear flaps (Cocker Spaniels, Basset Hounds, Bloodhounds) have reduced airflow in the ear canal, which compounds the problem. Breeds with a higher genetic predisposition to atopic dermatitis (Labrador Retrievers, Golden Retrievers, West Highland White Terriers, Bulldogs, German Shepherds, Boxers) are more likely to develop food-related ear disease.
If your dog is one of these breeds and has recurring ear infections, a dietary investigation is particularly worthwhile.
What Tracking Actually Shows You
Without tracking, an elimination diet produces a general impression — "I think the ears have been a bit better." With tracking, you get data.
Over 8 to 12 weeks of daily records, patterns emerge that are invisible to casual observation:
- A gradual decline in ear symptom severity scores that week-to-week feels imperceptible but over two months is clear.
- A spike in ear symptoms 4 days after an accidental exposure to a trigger protein — confirming the connection.
- The specific week during reintroduction when chicken was added back and ear redness returned within 5 days.
- The fact that venison has been fed for 3 weeks with zero ear symptoms — establishing it as a safe protein.
- Seasonal overlap: environmental pollen producing mild symptoms in spring that are distinct from the year-round pattern caused by food.
This is the difference between guessing and knowing. And for a dog who has been through multiple rounds of ear infections, antibiotics, and antifungals, knowing is worth the effort.
Your Dog's Ears Are Trying to Tell You Something
Recurring ear infections are not random bad luck. They are a signal — often a signal that something in your dog's daily diet is driving chronic, low-grade inflammation that creates the conditions for infection to take hold, again and again.
The infections need treatment. But the pattern needs investigation.
A structured elimination diet, maintained for the full recommended duration and tracked consistently throughout, is the most reliable way to determine whether food is the driver. It requires patience and discipline. But the potential outcome — breaking a cycle that has been causing your dog discomfort for months or years — is significant.
Your dog cannot tell you what's causing the problem. But with the right approach and consistent data, their body will show you.
Data Sources
- Olivry T, Mueller RS. Critically appraised topic on adverse food reactions of companion animals (2): common food allergen sources in dogs and cats. BMC Vet Res. 2016;12:9.
- Hensel P, Santoro D, Favrot C, Hill P, Griffin C. Canine atopic dermatitis: detailed guidelines for diagnosis and allergen identification. BMC Vet Res. 2015;11:196.
- Nuttall TJ, et al. Update on pathogenesis, diagnosis, and treatment of atopic dermatitis in dogs. Vet Dermatol. 2012;23(4):268-79.
- Angus JC. Otic cytology in health and disease. Vet Clin North Am Small Anim Pract. 2004;34(2):411-424.
- Olivry T, et al. Critically appraised topic on adverse food reactions of companion animals (1): duration of elimination diets. BMC Vet Res. 2015;11:225.
- Mueller RS, Olivry T. Critically appraised topic on adverse food reactions of companion animals (4): can we diagnose adverse food reactions in dogs and cats with serum IgE and IgG? BMC Vet Res. 2017;13:275.
- Tham HL. Elimination Diet Trials: Steps for Success and Common Mistakes. Today's Veterinary Practice. 2024.
- Verlinden A, et al. Food allergy in dogs and cats: a review. Crit Rev Food Sci Nutr. 2006;46(3):259-273.
- Olivry T, Mueller RS. Critically appraised topic on adverse food reactions of companion animals (9): the most common food allergens in dogs and cats. BMC Vet Res. 2019;15:349.
Disclaimer: This article is for educational purposes only and does not constitute veterinary advice. Always consult with a qualified veterinarian before changing your dog's diet or stopping any prescribed treatments. Recurring ear infections can have multiple causes requiring specific veterinary diagnosis and treatment. Active ear infections require veterinary treatment; do not attempt to manage them with diet alone. This article does not replace a professional veterinary examination.